BY KATE SERODIO, DPT/OWNER Unlike The Commonwealth Motors slogan “shop us last”, Physical Therapists across the nation are trying to educate everyone on shopping PT first! The goal is to inform and educate the benefits of Physical Therapy (PT) for both your injuries...
Blog
30 Reasons To Choose Hampton Physical Therapy!
Actually, There are 30 GREAT Reasons To Choose Hampton Physical Therapy! 1. ALL practitioners have Doctorates of Physical Therapy 2. Treating and supporting Hampton & Seabrook (Seacoast) community for 15yrs! 3. No aides or assistants, your care is from a Doctor of...
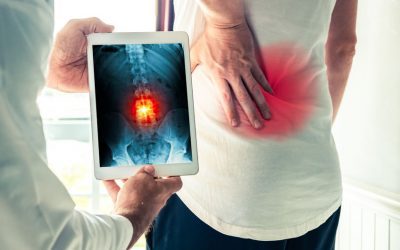
Low Back Pain and Imaging Explained
By Jess Leberman, DPT – Hampton Clinic ~ Low back pain (LBP) is a significant condition in the general population making it the leading cause of daily activity and work related limitations and absences. It is estimated the lifetime prevalence of non-specific low back...
Hampton Physical Therapy Clinics Now Certified in Blood Flow Restriction Training
Hampton Physical Therapy, with clinics in both Hampton and Seabrook, NH is proud to announce that all of their therapists have received certifications in Blood Flow Restriction "BFR" Training . Blood flow restriction training is a method of strength training that...
Wishing All a Joyful Holiday Season!
Wishing all our patients and friends the merriest and healthiest of holidays!
2nd Annual PLANK TIL YOU TANK at WHS
Winnacunnet HS Student Athletes Compete in 2nd Annual Hampton Physical Therapy 'PLANK TIL YOU TANK' Challenge Kicking off the Columbus holiday weekend, on Friday, October 5th, Hampton Physical Therapy’s exciting 'Plank Til You Tank' challenge was held for the second...
Shoulder Dislocation – Types and Treatments
By Michael Brezak, DPT – Hampton Physical Therapy, Hampton NH Clinic - There are many different types of joints in the human body. Some are more fixated while others tend to have higher mobility. This of course comes at a cost as the joint with higher degrees of...
Dizziness & Vertigo ~ PT Can Help!
By Lisa Wheldon, DPT, Hampton Physical Therapy - Seabrook NH Clinic Have you ever rolled over in bed and suddenly the room starts spinning? Maybe you went to get your hair done at the salon and you tipped your head back in the sink and you became nauseated. Or every...
Are Shin Splints Wrecking Your Run?
Physical Therapy Can Help! By Jessica Leberman, DPT – Hampton Clinic Medial Tibial Stress Syndrome (MTSS) more commonly referred to as “shin splints” is an injury of the lower leg that primary occurs in the exercising population1. MTSS makes up to 16% of injuries that...
How Stretching Will Improve Your Life!
By Kate Serodio, DPT From childhood, we've all been reminded to sit up tall, not slouch, stretch, and pull your shoulders back for good posture. If you engage in a sport or even go for a walk, it has embedded in your mind “make sure you stretch before, after, and...
Send Us A Message
Locations
Hampton Clinic
Hampton, NH, 03842
Mon-Thu 7am-7pm - Fri 7am - 6pm
Hampton South Clinic
Seabrook Clinic
920 Lafayette Rd (Route 1) Unit 2 (second floor of Seacoast Sports Club)
Seabrook, NH, 03874
Mon-Thu 7am-7pm - Fri 7am - 6pm