by Jessica Leberman, DPT – Hampton NH Clinic
by Jessica Leberman, DPT – Hampton NH Clinic
- Young athletes may have had an increase in complaints of knee pain this past winter after playing on harder indoor courts. Adolescent athletes are among those most frequently plagued by knee injuries. Knee pain and clicking not precipitated by a traumatic injury is a common complaint heard from young athletes. One of the most common diagnoses for adolescents with knee pain is Patellofemoral Pain Syndrome (PFPS)(1).
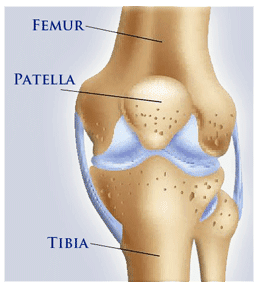
The knee joint is comprised of the articulation of 3 bones; the femur, the tibia and the patella (knee cap). The patella rests in a groove commonly referred to as the “patellar groove”. As a person bends and straightens the knee the patella glides within the groove(1).-
What is Patellofemoral Pain Syndrome?
- PFPS is an umbrella term used to describe pain and/or clicking or crunching in and around the knee joint associated abnormal gliding of the patella in the patellar groove. Often the symptoms occur on the front side of the knee and underneath the patella.
- Common signs and symptoms of PFPS include;
• pain with repetitive activities such as running, jumping, or squatting
• pain with climbing/descending stairs
• pain after sitting with your knees bent for a long period of time such as in school at a desk, at the movie theater or on an airplane
• Popping or crackling sounds (known as crepitus) in your knee when bending the knee or squatting down(1)
What Causes Patellofemoral Pain Syndrome?
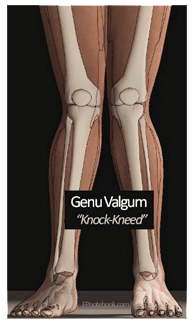 Common causes of PFPS include a change in activity level, a change in activity surface, or a change in footwear. Adolescents that participate in activities on more firm surfaces such as basketball, indoor track and dance are more prone to PFPS. PFPS can be due to abnormal alignment of the patella within the patellar groove, muscle imbalances, biomechanical abnormalities of the hip, knee and/or feet, and walking/running/jumping mechanical faults1. Genu valgum (knock knees) is a biomechanical abnormality commonly associated with PFPS. PFPS occurs more commonly in females (55%) than males (45%) as females are more prone to genu valgum(2).
Common causes of PFPS include a change in activity level, a change in activity surface, or a change in footwear. Adolescents that participate in activities on more firm surfaces such as basketball, indoor track and dance are more prone to PFPS. PFPS can be due to abnormal alignment of the patella within the patellar groove, muscle imbalances, biomechanical abnormalities of the hip, knee and/or feet, and walking/running/jumping mechanical faults1. Genu valgum (knock knees) is a biomechanical abnormality commonly associated with PFPS. PFPS occurs more commonly in females (55%) than males (45%) as females are more prone to genu valgum(2).
How can Physical Therapy help?
A physical therapist will perform a full assessment to determine the underlying source of your pain and establish a comprehensive individualized plan based on your presentation. Your individualized plan can include any combination of the following;
• Taping treatments to address mal-tracking of the patella(3)
• Guided strengthening activities of the core, pelvic, hip, knee and ankle stabilizing muscles(4)
• Myofascial treatments such as stretching, Instrument Assisted Soft Tissue Mobilization and Dry Needling.(5)
• Assessment for orthotic prescription to address abnormal biomechanics of the feet. Those who over pronate (more commonly referred to as having flat feet) are more prone to PFPS and can benefit from arch support in shoes.(6)
• Assessment of your walking, running, and/or jumping mechanics and training to optimize mechanics and dynamic balance to decrease abnormal stresses through the knee joint.(4,6)
Although adolescent athletes are those that frequently experience PFPS people of any age and activity level can experience symptoms related to PFPS. If you start to notice knee pain or crepitus within your knee Hampton Physical Therapy can help you. If you have any questions regarding this condition feel free to call or stop into one of our two locations in either Hampton or Seabrook to speak to one of our physical therapists.
References:
1. Patellofemoral Pain Syndrome-OrthoInfo–AAOS. https://orthoinfo.aaos.org/topic.cfm?topic=A00680
2. Glaviano NR Kew M Hart JM Saliba S. Demographic and epidemiological trends in patellofemoral pain. Int J Sports Phys Ther. 2015;10(3):281-290
3. Kurt EE, Büyükturan Ö, Erdem HR, Tuncay F, Sezgin H. Short-term effects of kinesio tape on joint position sense, isokinetic measurements, and clinical parameters in patellofemoral pain syndrome. J Phys Ther Sci. 2016 Jul;28(7):2034-40
4. Chevidikunnan MF, Al Saif A, Gaowgzeh RA, Mamdouh KA. Effectiveness of core muscle strengthening for improving pain and dynamic balance among female patients with patellofemoral pain syndrome. J Phys Ther Sci. 2016 May;28(5):1518-23.
5. Telles G, Cristovão DR, Belache FA, Santos MR, Almeida RS, Nogueira LA. The effect of adding myofascial treatments to an exercise programme for patients with anterior knee pain. J Bodyw Mov Ther. 2016 Oct;20(4):844-850
6. Powers CM. The influence of altered lower-extremity kinematics on patellofemoral joint dysfunction: a theoretical perspective. J Orthop Sports Phys Ther. 2003 Nov;33(11):639-46.